Whether it’s for a routine screening or for follow-up care, making sure a patient shows up to their appointment is critical to them living a healthy life. However, despite how important it is to seek care, especially in the case of recovery, some patients struggle to remember to attend their appointments. In fact, even if an appointment is scheduled during the discharge process, no-show rates exceed more than 50% as patients forget to attend. This can have significant implications not only for a patient’s health but also for a healthcare organization’s bottom line.
One solution is implementing appointment reminders. They have been shown to effectively reduce no-show rates, and by extension, reduce readmissions and improve patient outcomes. And in a time when resources are tough, relying on technology, like CipherOutreach, to do the work and send automated calls or reminder texts to patients to confirm their appointments can significantly reduce the burden on staff.
So whether you’re considering implementing an appointment reminders program or you have one in place, here are five best practices to more effectively engage patients and ensure they show up to their upcoming appointment.
- Use shortcodes and a phone number your patients recognize: Before you even contact a patient, you need to consider the factors that might prevent you from reaching them. With all of us receiving several spam calls per day, you need to use a phone number that patients will recognize – or they won’t pick up the reminder call. Additionally, if you are contacting patients via text message, leverage SMS short codes. These codes allow you to send high volumes of messages that won’t get blocked by phone carriers.
- Keep in mind patients’ preferred languages and communication channels: Not every patient wants to pick up the phone and not every patient speaks English. In recognizing patients’ preferred language and communication channel, you can increase engagement and ensure patients get the information they need (e.g., pre-visit instructions) when they need it. For example, one of our customers, UC Irvine, added voice outreach to their SMS program and increased patient engagement by 20%. Accounting for patient preferences is also a way to improve the experience all patients have with your organization.
- Provide pre-visit instructions and safety information: Regardless of how often one goes to the doctor, healthcare can be confusing. This is especially true now as we continue to live through a pandemic. Using pre-visit communications to educate patients about your COVID-19 safety protocols, provide directions to your facilities, or answer questions can do a lot to reduce fears and provide clarity, leading to a better patient experience, which increases the likelihood patients will show up for their appointments.
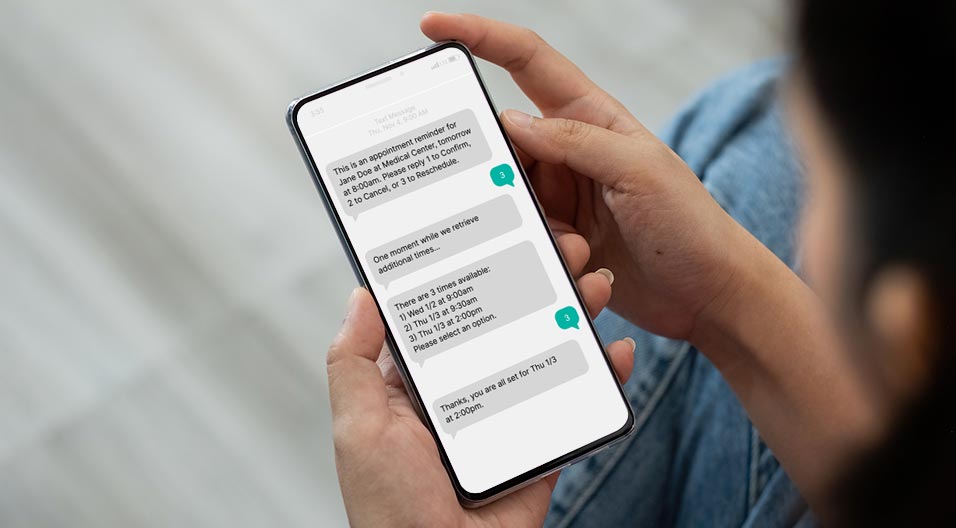
- Implement multiple reminders to confirm, cancel or reschedule: Reminding patients of an upcoming appointment – and doing so several times – is an effective tactic for reducing no-shows. It also provides an opportunity for you to backfill that visit when there is a cancellation by allowing patients to reschedule through self-service options, which won’t additionally burden your call centers. In implementing automated appointment reminders, our partner, Community Health Network, was able to retain $3M+ in revenue and decrease their no-show rate by 1.2%.
- Capture data and analytics to monitor your success: Gaining insight into how effective your pre-care outreach tools are is one of the best ways to improve engagement with patients. For many of our customers, we’ve recommended looking at reach rate, the number of patients who answer the calls (call vs. text and by department), and no-show rate in order to identify areas for operational improvements. Prioritizing these metrics enables you to identify issues and strategize ways to improve these numbers.
Learn more about our pre-care solutions and how they can help you proactively engage patients here.