Meet the patient rounding tool that revolutionizes patient care. CipherRounds enables purposeful rounding to help you improve communications, understand and address quality and patient safety issues as they happen, and use real-time actionable insights when it matters most.
CipherRounds™
Patient, Staff & Location Rounding Tool
Take the pen and paper out of patient rounds
Digitize rounding to improve patient care outcomes and enhance staff satisfaction – for happier, healthier patients.


Natalie Carr does not understand her discharge instructions and uses Self-Service Rounding to submit questions through her mobile device.The nursing staff receives an automated notification and spends extra time with Natalie and a family member before she goes home.
Connecting with your staff has never been more important. CipherRounds not only relieves hospital staff of manual tasks associated with traditional patient rounding, but it also gives leaders a rounding platform to have meaningful check-ins with their teams. Providers can recognize their colleagues, and patients can share their patient experience and appreciation for their clinicians.
Maximize rounding efficiency with CipherRounds
Watch Video
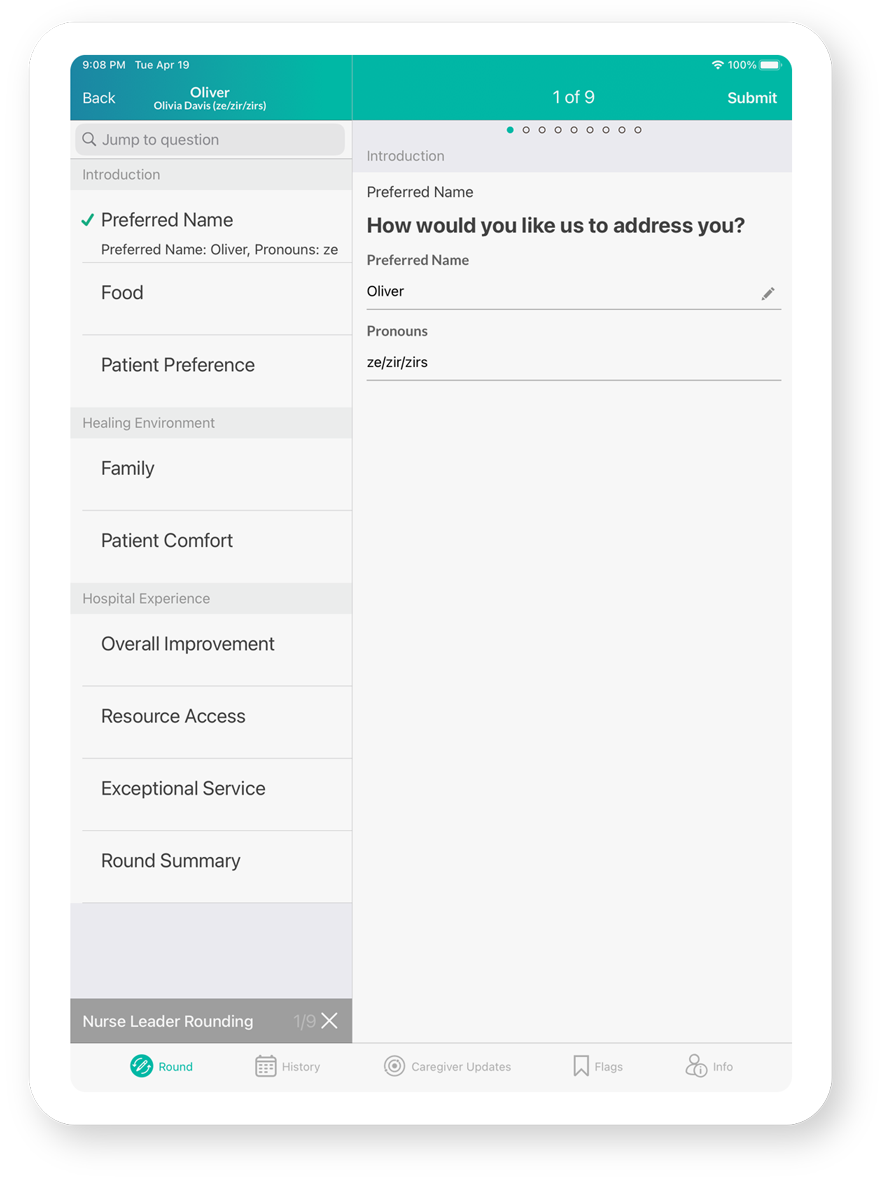
Capture Patient Pronouns
Demonstrate courtesy and respect by asking patients and staff how they would like to be addressed.
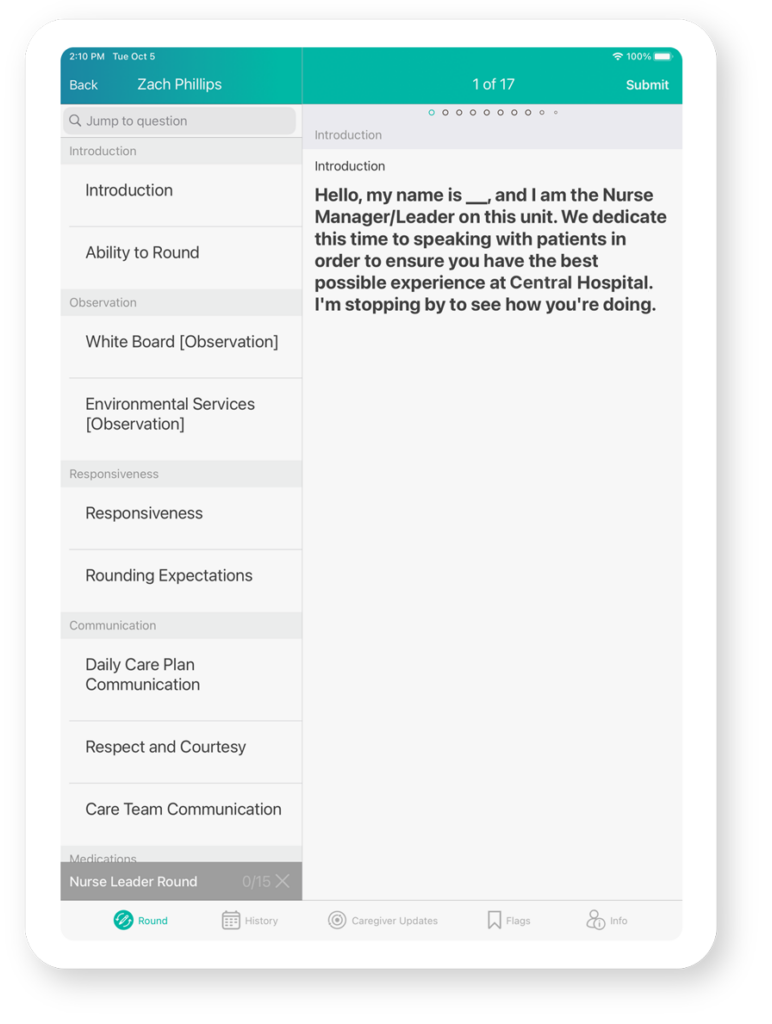
Give Patients Extra Attention
Show your organization’s commitment to providing quality care and increasing patient satisfaction through nurse leader rounding.
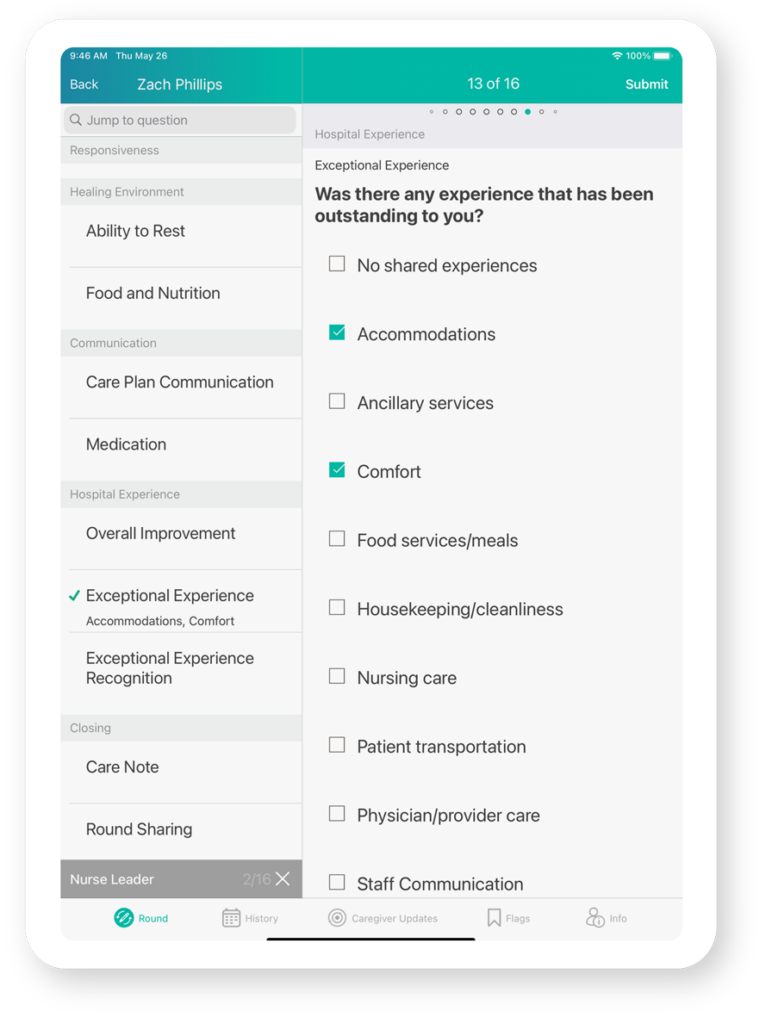
Survey Patients
Ask about patients’ experience in the hospital to find out what they enjoy and what areas remain for improvement.
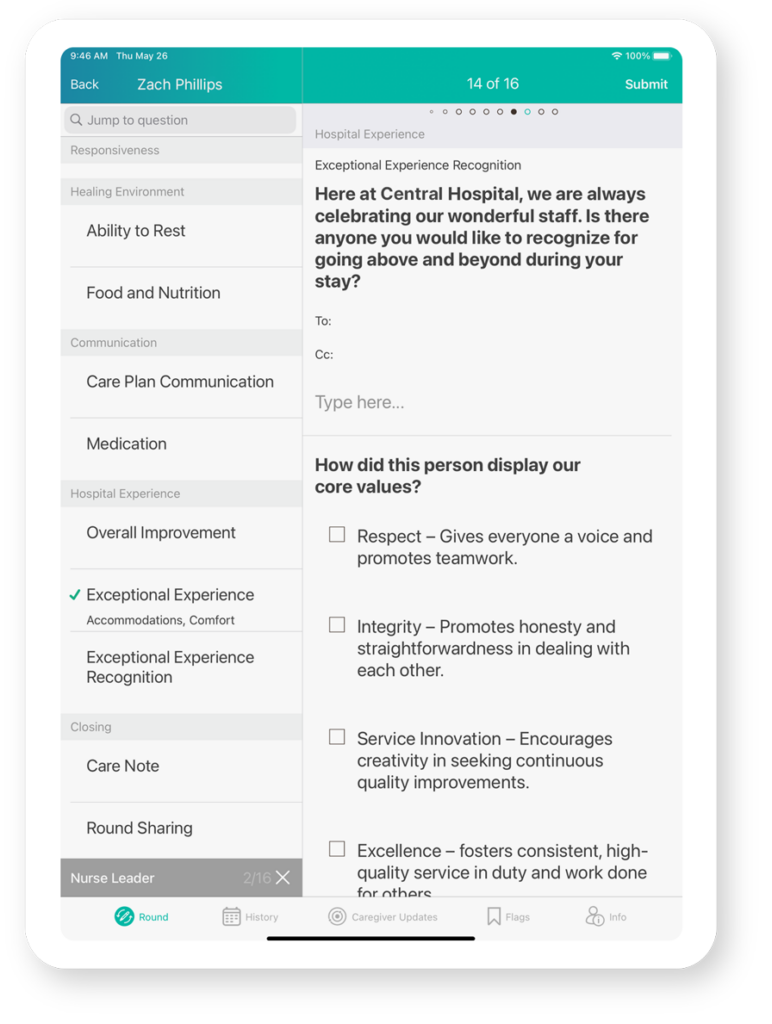
Celebrate Staff
Let patients and colleagues share the positive experiences they have with particular staff members. The feedback is shared with each individual and can be integrated into reward programs.
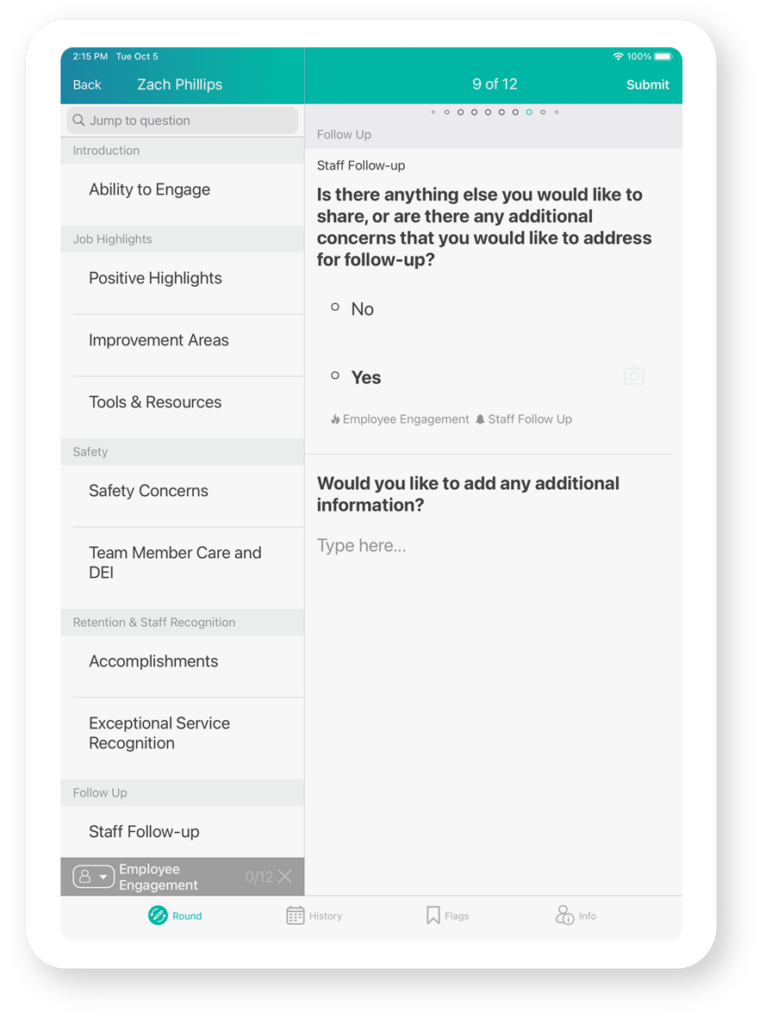
Check In With Your Staff
Foster trust by regularly touching base with your staff to find out their current concerns so you can work to address them.
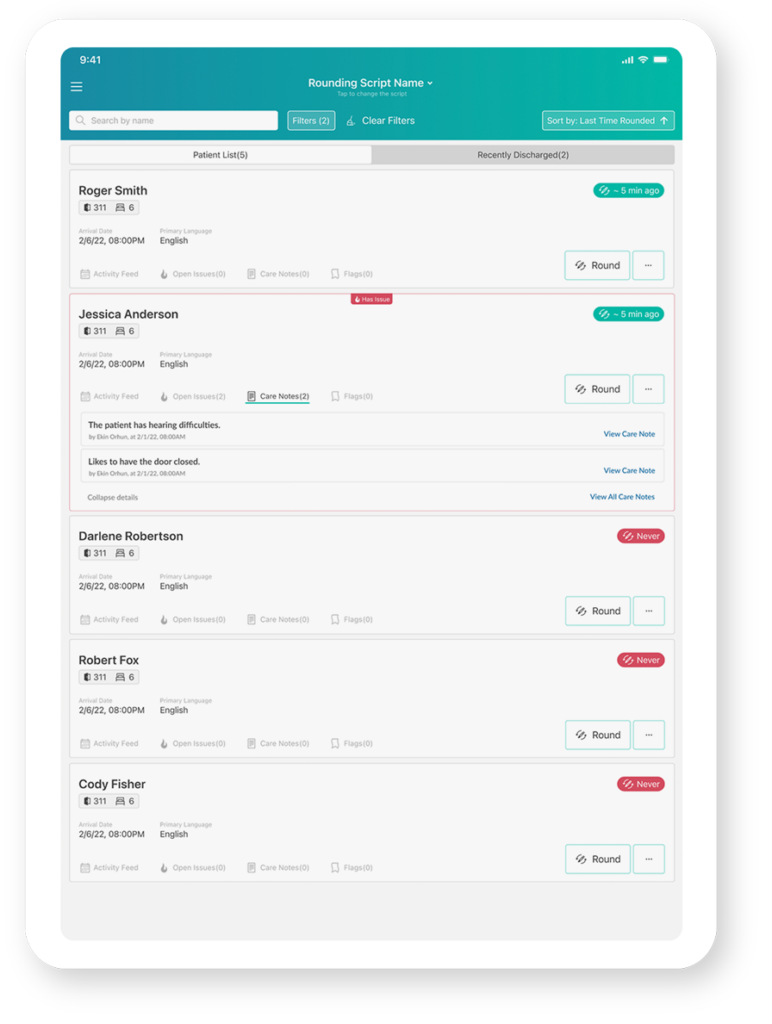
Efficiently Prepare for Rounds
Maximize your time with patients using straight-forward snapshots of patient data in a single view.
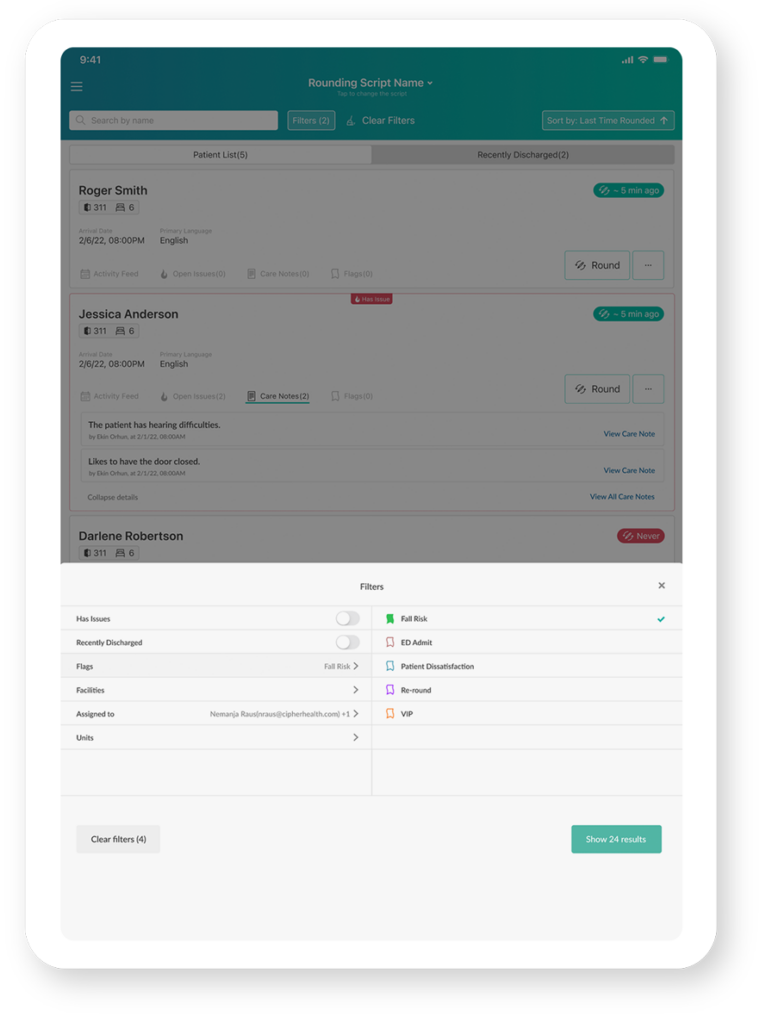
Customize Your View
Select filters to focus on the data you need most.
Drive Patient Loyalty
Give patients the control to provide feedback on their own through self-rounding, improving patient experience and building trust with the health system.
Reduce Manual Tasks for Staff
Empower patients to self-round, saving staff time so they can prioritize rounding efforts and connect with individuals based on their personalized responses.
Improve Continuity of Care
Review a timeline of essential patient movements and interactions at your health system to enhance communications and deliver more personalized care.
Power purposeful conversations with patients and staff
Akron Children’s Hospital scaled their rounding program across
100 locations in just 4 days
“
With CipherRounds, we are able to support nurse accountability for rounds, but even more importantly, we are providing the healthcare services patients and families need quickly.”
Joy Burt
Patient Experience Improvement Manager
Akron Children’s Hospital

CipherRounds improves the quality of interactions between patients and staff so care providers can give patients the personalized care they deserve – and leaders can better support their staff.
Improve patient outcomes
Use physician and nursing staff alerts to quickly resolve clinical issues and notify case managers for questions prior to discharge.
Increase patient satisfaction
Create meaningful interactions that show patients you care about their needs and preferences, and alert patient advocates if patients have questions about their care.
Promote staff well-being
Foster a culture of open communication, promote coordination among care teams and make necessary changes to optimize workflows.
Drive lasting quality and safety changes
Proactively manage compliance and safety checks among hospital staff, patients and the environment of care.
Achieve excellence through insights
Establish best practices in your scripts, and leverage in-depth reporting to pinpoint trends and improve patient outcomes.




Tracked over
and completed 3.7M rounds on 1.6M patients
Captured
with 60k ideas for improvement were shared with leadership
Provide the care your patients expect and keep your staff happy








