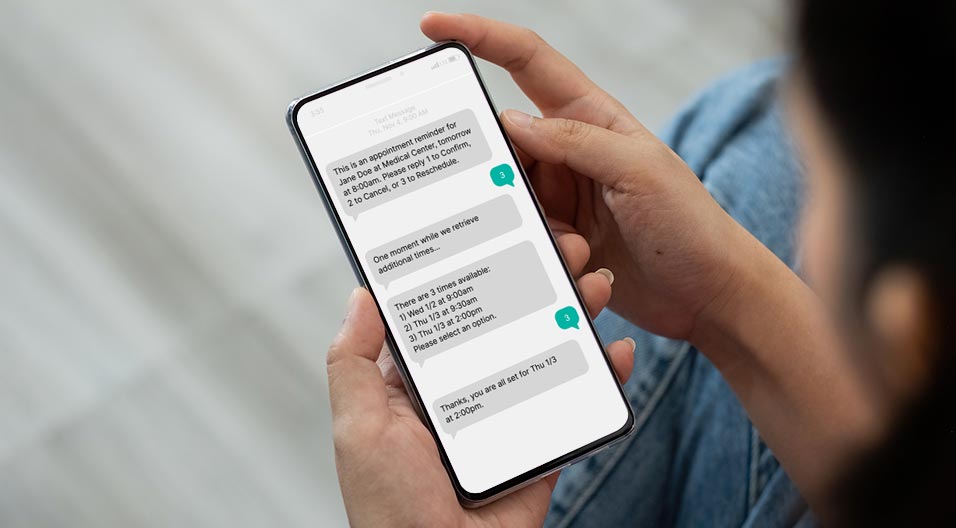
It’s 2019 and chances are your physician practice is using an automated patient reminder platform for appointment reminders, and for good reason. MGMA estimates that practices have an average no-show rate of 5-7 percent, and this translates to lost revenue, inefficient schedules, and negative outcomes, especially for chronically-ill patients.
For many practices, however, this is where automated patient reminders start and end. While taking proactive steps to reduce patient no-shows is important, it’s only one piece of the larger equation. To maximize the potential of your patient outreach program, your practice needs to create meaningful, consistent, and timely interactions with patients across their care journeys, not just before their appointments. Leveraging the right technology can help you scale these efforts with minimal labor required.
Help Your Patients Embrace Prevention
As the healthcare industry slowly marches toward value-based care, providers are increasingly being incentivized for their patients’ use of preventive care services and must report on quality measures that are tied to reimbursements. This makes good sense – patients who take preventive measures today will likely be healthier (and less costly to care for) tomorrow.
While most patients understand this logic, many don’t follow through. In fact, studies have shown that Americans use preventive services at about half the recommended rate.
There are certainly a number of factors that can impact the likelihood of patients skipping out on preventive care. Social determinants of health, high deductibles, and copayments, amongst other factors, are all legitimate barriers to care. Even the patients who have the resources and best intentions often forget to schedule their routine colonoscopies, mammograms, and wellness visits.
This presents a significant opportunity area for physician practices to better leverage automated patient reminders. Rather than waiting to discuss preventive care during sick visits or for patients to make the first move, physician practices can gently remind patients who will soon be due for preventive care services and give them an easy way to schedule these appointments. By integrating reminder tools with EMRs or registry systems, providers can easily identify soon-to-be gaps in care and deploy targeted reminder campaigns to proactively narrow them.
UCSF Health is one example of a healthcare organization that has achieved considerable success with preventive care reminders. The health system participates in a number of value-based programs that require them to prioritize population health management. By using automated patient reminders, UCSF has been able to surpass quality measure performance targets, and has tripled key cancer screening rates (colorectal, breast, and cervical) and increased flu immunization walk-ins by 38% across their outpatient clinics.
Position Patient Care Transitions for Success
If you’re part of one of the many physician practices that’s affiliated with a local health system or hospital, there’s also an opportunity for your organization to use automated patient reminders to help optimize care transitions.
In recent years, providers across the continuum have been forging partnerships to enhance care coordination efforts and guide the appropriate utilization of healthcare services for their patient populations. There has been a notable uptick in the number of physician practices that are outright owned by hospitals, and both acute and ambulatory care now have a shared responsibility to keep their patients healthy in their communities.
This is especially true for patients transitioning from an acute care setting to home. During this very sensitive time period, providers must ensure that patients have an adequate understanding of their care instructions and necessary care team follow up to help keep them on the path to recovery.
Following an inpatient stay or Emergency Department (ED) visit, patients are no longer under the 24/7 care of healthcare professionals and are required to manage their care plan on their own. Given the many social factors at play that can potentially get in the way of a patient’s recovery, post-discharge outreach is a proven strategy to help increase the chances of a smoother transition of care. Automated outreach tools can enable healthcare organizations to reach all patients transitioning between settings and mitigate negative health outcomes.
For example, Choptank, a Federally Qualified Health Center (FQHC) that’s part of the Maryland Community Health System, needed to find ways of providing more effective follow up to patients leaving the hospital and ED. The organization decided to integrate an automated patient reminder platform with Maryland’s State Health Information Exchange (HIE) to send timely outreach to recently discharged patients. As a result of the outreach program, Choptank had a 37 percent decrease in 30-day readmissions and 38 percent decrease in ED returns. The use of automated follow up calls guide patients toward PCPs and other community resources within the system for follow up care, contributing to the program’s success.
Help Your Patients Help Themselves
As outcomes increasingly become a key performance driver for your physician practices, developing strategies to proactively engage patients not just before, but after and in between visits becomes more and more critical. Automated patient reminders is a proven, cost-effective way for your organization to scale its outreach efforts without having to utilize valuable staff time, and truly helps to put your patients in the driver’s seat and take control of their health.
Want to dig deeper? We invite you to check out these additional resources that explore how automated patient reminders can be used across care journeys: