In this series, we explore the concept of Patient Experience as an outcome measure and Patient Engagement as the Strategy that healthcare organizations and providers take to positively impact the Patient Experience. In this article, we highlight how post-discharge follow up provides the opportunity to close the loop and maximize the patient experience beyond the four walls of the hospital.
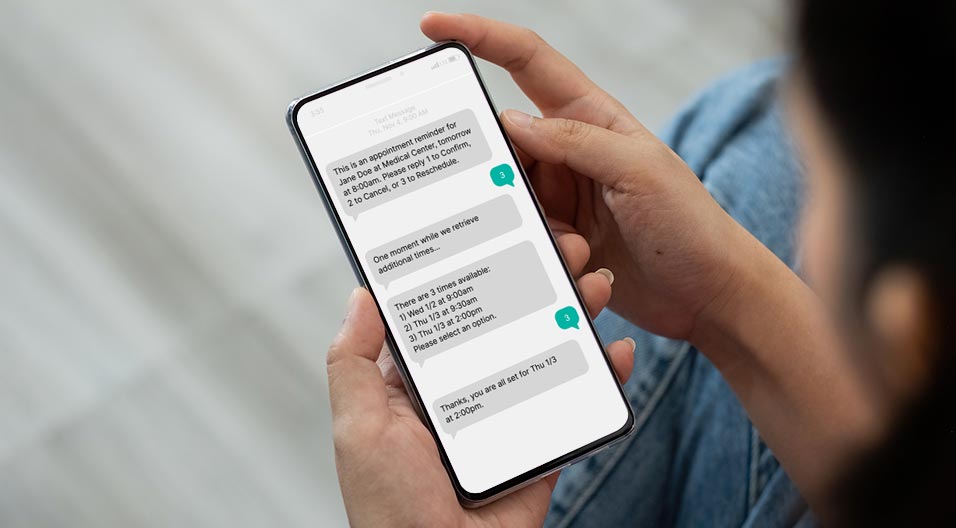
Given that we have explored that an effective patient engagement strategy needs to meet the patient at the point they are at in their care journey, it is crucial to explore how providers can continue to deliver exceptional care during the post-discharge period. Every patient deserves timely follow up and hospitals cannot afford not to make post discharge follow up a key part of their strategic plan. The consequences of not extending your patient engagement strategy outside of the four walls are dire; and include poor patient clinical outcomes, reduced patient satisfaction, and 30-day readmissions. There are so many examples of patients needing additional assistance and proactive outreach is a key part of a patient engagement strategy to prevent harm and increase patient satisfaction. Providers who enable post-discharge engagement have the opportunity to perform service recoveries prior to the HCAHPS survey being completed, and more importantly, can prevent adverse events such as a readmission from occurring.
Automated Outreach is a Valuable Asset for Engaging Patients
More often than not, providers are unable to find the dedicated resources to manually reach out to all of their patients post-discharge. If there are dedicated resources, they may only focus on a small subset of patients, typically those perceived to be the highest risk. While this is certainly better than no patients receiving follow up, every patient (with some exclusions), especially those discharged to home, should receive a follow up call.
Even with fully staffed call centers, it can be challenging to ensure there is consistent outreach to every patient, not to mention ensuring they receive a call back if they don’t answer the first call. This is where automated outreach proves to be an extremely powerful engagement tool. With technology, hospitals can reach out to 100% of patients, and do so multiple times throughout the 30-day window. There is no chance that someone forgets to try a call-back if unable to reach the first or second time. By engaging patients during this critical time post-discharge, the organization shows its dedication to ensuring a safe transition.
Follow up not only makes patients feel more confident in their care, but it provides the opportunity to perform any service recovery. If a patient had a negative interaction or is unsure about their discharge instructions, the follow up interaction can help resolve the concern and proactively address the issue. This is an important part of an effective patient engagement strategy and sometimes addressing an issue after discharge happens at the right time and is essential in keeping patients satisfied with their care.
Post-Discharge Follow Up in Action: How Upstate University Hospital Improves Outcomes and Experiences with Centralized Outreach
Upstate University is an academic medical center based in New York. As a large healthcare provider, it was critical to find an efficient process for post-discharge follow up. By creating follow up efficiencies, Upstate knew they could positively impact readmission rates. In addition to improving patient outcomes, the medical center also saw the follow up process as a way to ensure patients were satisfied with their care.
To maximize resources, Upstate put in place a centralized team responsible for all post-discharge follow up. By combining the dedicated resources with CipherOutreach for inpatient follow up, the team was able to address patient-reported issues quickly and effectively. This quick response time and proactive outreach led to multi-year improvements in both readmission rates and HCAHPS scores, indicating the positive impact this engagement has on patient experiences.
With incentives tied to both patient satisfaction scores and readmission rates, proactive follow up is a proven engagement strategy that can help maximize these incentives. By providing timely follow up, your organization can truly show the dedication to providing high-quality care and drive improved loyalty. If you would like additional information, I invite you to read the full case study and uncover the process that Upstate followed to achieve positive outcomes and experiences for their patients year over year.